[tldr]
- If you’ve been on hormonal birth control, you might be concerned about things like cancer risk, estrogen dominance, and sex drive.
- From disposable methods like condoms and sponges, to reversible methods like the IUD, to permanent sterilization, you have several birth contraceptive options that won’t mess with your hormones.
- If you’re ready to reset your body without giving up sexy time with your partner, keep reading to learn about your non-hormonal birth control options and the pros and cons of each.
[/tldr]
You may have landed here because you’ve been learning about how hormonal birth control affects you with long-term use. If you’ve been on hormonal birth control like the Pill, you might be concerned about things like:
- Skin changes
- Breast changes
- Long-term cancer risk
- Estrogen dominance
- Hair loss
- Libido
There’s so much more than that. For more detail, this podcast episode of Bulletproof Radio with women’s health expert Sarah Hill, PhD (iTunes) explains the mess that hormonal birth control makes in women’s bodies, head to toe.
If you’re ready to reset your body without giving up sexy time with your partner, keep reading to learn about your non-hormonal birth control options and the pros and cons of each.
Types of non-hormonal birth control methods
Hormonal contraceptives are by far the most popular methods of birth control. You might be surprised at how many non-hormonal options are out there, like:
- Male condoms
- Female condoms
- Sponge
- Diaphragm/cervical cap
- Spermicide
- Copper IUD
- Rhythm method
- Tubal ligation
- Vasectomy
- Withdrawal
- Herbal birth control
- Wild carrot seed
- Smartweed
Here’s the rundown on each, and what to expect using each method.
1. Male condoms
Effectiveness*: 98% effective with perfect use, 85% effective with typical use
Male condoms are a thin balloon-like sheath, usually made of latex, nitrile (synthetic latex), or less commonly animal skin. They’re cheap, easy to carry with you, and widely available in grocery stores and pharmacies. When you use them correctly, they’re an effective contraceptive.
There are a few downsides, though. A biggie is that you have to have them on-hand before you need one, whether you’re home or away from home. Sometimes those moments sneak up on you when you least expect it, so you have to be prepared. Especially when you’re tipsy, you’re more likely to forget.
Another downside is that condoms aren’t medicine and they’re not food, so the government doesn’t require manufacturers to label what’s in them. A lot of condoms contain toxins, allergens, and hormone disruptors, and given their point of contact, you could end up with infections, reactions, or hormone problems in your delicate reproductive system. Your body might detoxify brief exposure here and there without too much trouble, but if condoms are your go-to method, these chemicals will compound over time.
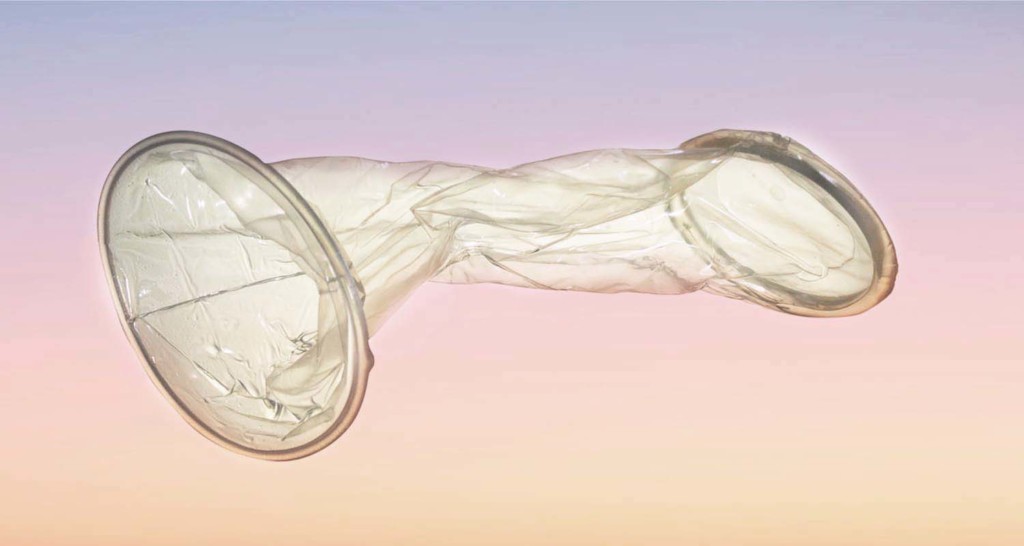
2. Female condoms
Effectiveness: 95% effective with perfect use, 79% effective with typical use
Female condoms look like a larger male condom with a small ring at the closed end and a larger ring at the open end. They stay in place surprisingly well and provide all of the same benefits as the male condom.
You’ll run into all of the same issues that you have with male condoms, like the chemicals they’re made from and having them on hand when you need them. A few extra things to keep in mind include:
- Availability. Female condoms are a little harder to find than male condoms, so a spontaneous grab-and-go might not be an option depending on where you are.
- You need a dry run (no pun intended). It’s best to practice inserting one before you need it, because getting it right can be tricky at first.
Some couples prefer female condoms to male condoms because of the extra stimulation the rings provide.
3. Spermicide (nonoxynol-9)
Effectiveness: 82% effective with perfect use, 72% effective with typical use. People usually use spermicide in combination with a barrier method to increase the effectiveness of both.
Spermicide comes in lubricants, gels, or foams, and it works as a partial barrier by two mechanisms:
- It coats the cervix, blocking sperm
- It slows down, stops, or kills sperm before they can cross the cervix and reach the egg
Spermicide comes infused in other barrier contraceptives like condoms and the sponge; it’s recommended for use with others like the diaphragm; or you can use it on its own. Nonoxynol-9 is a detergent, so it erodes cell membranes. That’s all well and good when sperm are the targets, but it also disrupts the cell membranes of everything in its path, including healthy cells. Weakening your own cells increases your risk of genital lesions and sexually transmitted infections including HIV.[ref url=”https://www.sciencedirect.com/science/article/pii/S0140673602110798″][ref url=”https://jamanetwork.com/journals/jama/article-abstract/398713?redirect=true”]
The risk of infection seems to depend on frequency of use — the more you use it, the weaker your epithelium (the outer layer of your cells) becomes,[ref url=”http://europepmc.org/abstract/med/1658953″] and the higher your risk of infection.[ref url=”http://www.who.int/mediacentre/news/notes/release55/en/”] It also disrupts vaginal bacterial flora, which increases your risk of vaginosis[ref url=”https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1380307/”] and other microbiome imbalances.
There’s also concern that it’s a pesticide, so once it rinses away and makes it into the water supply, it can mess with the aquatic ecosystem. As with a laundry list of other pesticides, it has endocrine activity that can cause you hormone problems with repeated use.[ref url=”https://www.ncbi.nlm.nih.gov/pubmed/9342079″]
All you need to know: spermicide is nasty.
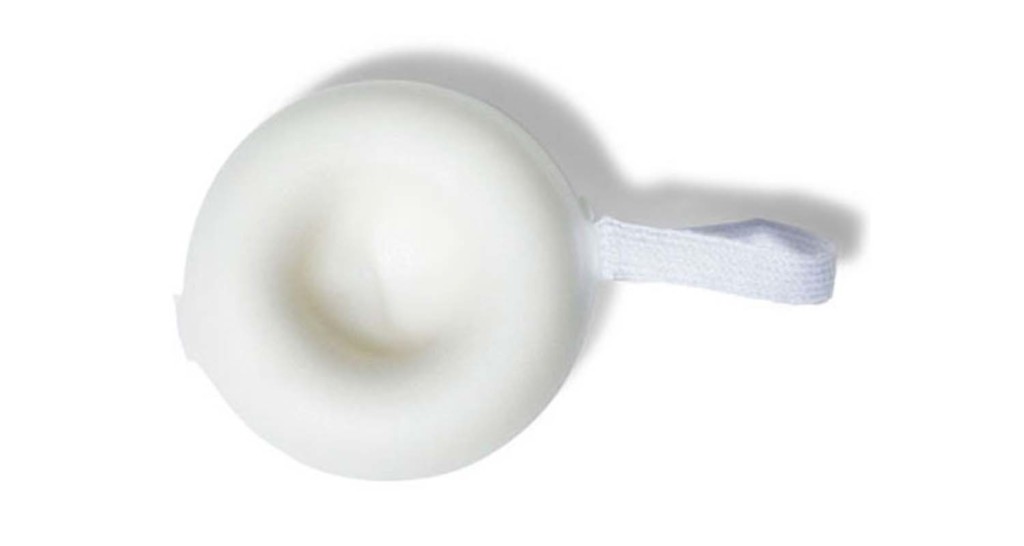
4. Contraceptive sponge
Effectiveness: 91% effective with perfect use and if the woman has never given birth; effectiveness declines with typical use and if the woman has given birth, down to 76% effective at preventing pregnancy.
The birth control sponge is a disposable squishy foam disc that contains spermicide, so it provides both a barrier to block the transfer of sperm, and it slows the sperm that come into contact with it so it doesn’t make it to the egg. You can wear it for up to 24 hours, so if you plan ahead, you don’t have to stop in the middle of everything to deal with it.
There have been reports of sponge users developing toxic shock syndrome (TSS), but the sponge was either left in too long or the user had difficulty removing it resulting in fragments left behind after removal.[ref url=”https://www.cdc.gov/mmwr/preview/mmwrhtml/00000273.htm”] TSS is rare, though.
The main problem with the sponge is that it contains spermicide, which you can read about above. That’s not something you want anywhere near your reproductive parts.
5. Diaphragm, cervical cap
Effectiveness: 94% effective with perfect use, 88% effective with typical use
The diaphragm is most closely related to a menstrual cup. It’s a reusable flexible plastic shallow cup you use to cover your cervix and block the transfer of sperm.
You can insert it hours before sexual contact, so once you get the party started, you don’t have to stop. The diaphragm itself doesn’t affect your hormones, but you only get to max effectiveness levels when you use it with spermicide, and that comes with a whole bunch of problems.
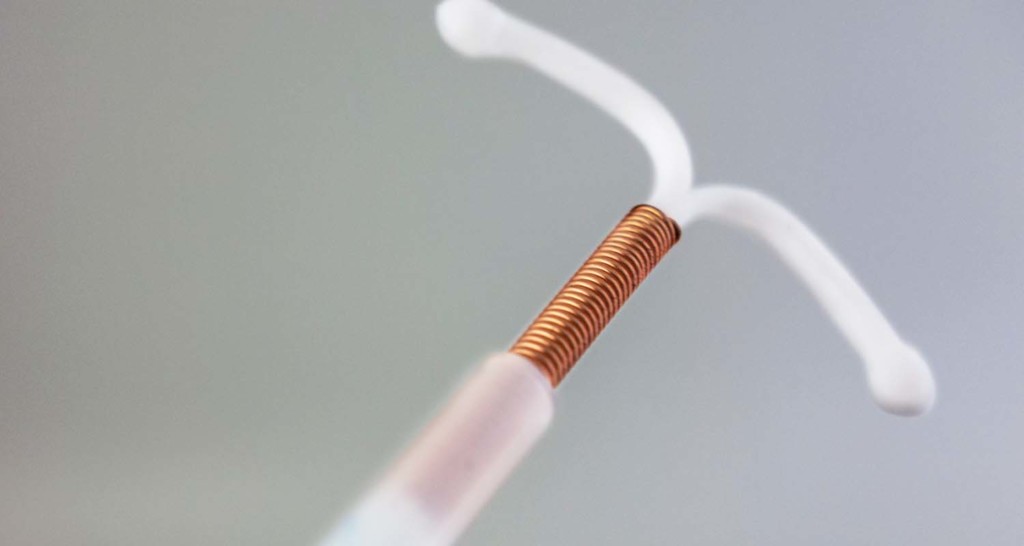
6. Copper IUD
Effectiveness: >99% effective at preventing pregnancy
The copper IUD is almost as effective as permanent sterilization, and you can reverse it at any time. With the copper IUD, you don’t get any synthetic hormone. There’s a small risk that it will fall out or go where it shouldn’t, and a handful of other risks, but they’re rare.
You don’t have to remember to take a pill every day or deal with your birth control right before or during sex. The copper IUD is a set-it-and-forget-it birth control method that you can keep in place for over a decade.
On the flipside, the constant exposure to copper stacks on top of your other everyday sources of copper like plumbing, pots and pans, and other sources, could lead to copper toxicity. If your copper balance tips, you could end up with things like:
- Fatigue
- Super heavy periods
- Excess estrogen
- DNA damage[ref url=”https://www.ncbi.nlm.nih.gov/books/NBK225400/”]
- Digestion problems[ref url=”https://www.ncbi.nlm.nih.gov/books/NBK225400/”]
- Liver scarring[ref url=”https://www.ncbi.nlm.nih.gov/books/NBK225400/”]
The levels in the IUD aren’t likely to cause copper toxicity alone, but if your exposure is already high, it can push you over the edge.
7. The fertility awareness method (aka rhythm method)
Effectiveness: varies
The fertility awareness method, aka natural family planning (NFP) or the rhythm method, involves being aware of your body’s changes throughout the menstrual cycle and predicting ovulation using your body’s biological changes.
Effectiveness depends on the method, and how well you know your body’s fertility cycle. There are several ways to do it, each with its own margin of error, so it’s best to combine things to track:
- Calendar. With the calendar method, you count days to predict ovulation. Your reproductive system doesn’t know what day it is, and sometimes it won’t follow the rules. There are lots of factors that influence your menstrual cycle, like stress and toxic exposures.
- Cervical mucus. The cervical mucus method involves being aware of changes in your cervical mucus throughout the month and getting familiar with the thicker, more slippery texture that comes around ovulation time.
- Basal body temperature. The basal body temperature method involves charting your body temperature with a specialized thermometer several times per day. Most women see a small temperature increase (0.5-1 degree) right before ovulation. Of course, a fever or chronic medical condition will throw off your numbers.
With practice, most women get really good at predicting ovulation. Problem is, sperm can live inside the woman’s body for days, so that’s why the methods recommend a few extra days before and after ovulation.
If you adhere to a religion that forbids chemical or barrier birth control, the fertility awareness method gives you some amount of control as to how many kids you have and when.
Onto the downside. Fertility awareness takes a lot of work, and there’s a bit of a learning curve as you get to know your body. Not only do you chart your patterns around the time you have sex, you also track throughout the month to establish your body’s patterns. Also, male partners can’t really help their ladies here. It’s up to the woman to take her basal body temperature, check cervical mucus, and chart everything along the way.
A side benefit of putting in all that effort to track your cycle is that women do certain things better at various phases of the menstrual cycle, so you can give yourself some life advantages. For example, you’re more confident and outspoken around ovulation time, so schedule big presentations and negotiations for mid-cycle.
8. Tubal ligation
Effectiveness: 99% in the first year, during which your fallopian tubes could fuse back together. After that, docs consider you sterilized.
Tubal ligation, aka getting your “tubes tied,” is a permanent sterilization method that blocks the path of the egg through the fallopian tubes.
It involves either:
- Inserting a coil (Essure) into each fallopian tube, with the intention that your body will envelop them in tissue that will block the tubes
- Clamping off the fallopian tubes with clips
- Damaging a small section of the fallopian tubes
There are risks including infection from the procedure itself, ectopic pregnancy, and others.
Doctors will tell you that tubal ligation doesn’t affect your hormone levels, but due to decreased blood supply to the ovaries[ref url=”https://www.sciencedirect.com/science/article/pii/S0140673685922093″][ref url=”https://www.ejog.org/article/S0301-2115(01)00410-9/fulltext”] and damaged or removed receptor cells, some women anecdotally report menopause-like symptoms.
9. Vasectomy
Effectiveness: Close to 100% after 3 months.
Vasectomy is a permanent male sterilization. It’s a quick surgical procedure that involves cutting or blocking the vas deferens, the tubes in your scrotum that sperm travel through toward the exit. The procedure itself takes only a few minutes and recovery is quick, only a few days.
Vasectomy doesn’t change the ability to ejaculate, and it doesn’t change the physical quality of your semen at all, except that it will not have sperm in it.
Risks include pain, swelling, and infection at the site, similar to that of any surgery with a small incision. Rarely but possibly, the tubes can grow back together and reverse the procedure. Some men have concerns about testosterone, but hormone profiles follow normal patterns after vasectomy.[ref url=”http://europepmc.org/abstract/med/1116628″][ref url=”https://www.popline.org/node/482847″][ref url=”https://www.bmj.com/content/1/6010/621.short”]
10. Withdrawal
Effectiveness: 96% effective with perfect use, 78% effective with typical use.
The withdrawal method involves stopping intercourse right before climax and ejaculating outside the body.
The withdrawal method is hormone-free, chemical-free, and cost-free. Sounds like an appealing method, right?
Except, it’s really easy to oops this one. The man could be too wrapped up in the task at hand to remember to withdraw, or he could misjudge when he will finish. Both partners’ minds will be (and should be!) elsewhere, and it’s incredibly easy to forget.
Even if you remember every time, a few overachievers can creep out before the grand finale and result in pregnancy.
11. Herbal birth control
Effectiveness: Unknown. Varies by the plant used, and it’s not well researched.
Societies around the world use tradition-based herbal birth control to prevent pregnancy with success.
Wild carrot seed. Some societies use wild carrot seed, aka Queen Anne’s Lace, as a morning-after pill of sorts. Take a teaspoon right after funsies and every day for a week. It’s best to seek the guidance of a highly trained herbalist or naturopathic doctor. For one, you want to make sure your dosing and timing works with the rest of what’s going on in your body, so you’ll need a full consultation. More importantly, Queen Anne’s lace looks just like deadly hemlock, so it’s a terrible idea to look up a photo of it and go foraging.
Smartweed. Some cultures use a large amount (1 qt daily) of a strong tea of smartweed to prevent pregnancy. Traditions vary and it’s not well-researched, so this is another time you want to work with an herbalist to make sure you’re doing it right.
Spoiler alert: no one method is perfect, so use the information here to open up a conversation with your functional medicine doctor about the right method for you. While you’re at it, get some STI prevention advice, too. Can’t hurt.
*This article focuses on birth control only, so effectiveness pertains to pregnancy prevention only. STI prevention is not addressed in prevention statistics.